This article was written to complement the best breast pump review and the best bottle warmer review to provide guidelines for proper handling of breast milk.
Treat It Like Liquid Gold
There is a reason why breast milk is lovingly referred to as “liquid gold.” Nutritionally and immunologically, there is no contest as to the superiority of human breast milk over formula. Breast milk promotes a healthy infancy and lifespan for both mother and infant. Once a good latch and milk production are established, mom just needs to make sure that she is eating and drinking adequately as well as is physically present when her baby wants to nurse. No milk to warm and no bottles clean, right?
Well, not necessarily. Exclusive breastfeeding, particularly for a prolonged period, can not only be impractical but also impossible for many mothers due to realities of insufficient milk production or a return to work.
Expressing Breast Milk
Whether back to work or separate from baby for some much coveted “me time”, expressing breast milk is something that most mothers tackle to maintain the breastfeeding relationship. Breast pumps, particularly electric over manual, save tons of time and toil compared to hand expression. Even if you are using the best of the best electric pump, however, it is important to understand how to best handle expressed breast milk from pumping to storage to baby drinking in order to keep it free from bacterial overgrowth and to maintain its full nutritional and immunologic value.
Employed moms generally begin to pump one to two weeks before returning to work. It is a good idea to introduce occasional bottle feeding before you return to work to help your baby get used to taking a bottle (however, wait at least 3-4 weeks after birth before you try to introduce bottles). Make sure you follow your breast pump manufacturers cleaning instructions to assure your milk supply is safe and healthy for your baby.
A common practice among working Moms is to pump 3 times during an 8-hour work shift, or every 3 hours you are away from the baby. Ten minutes of pumping during breaks and 15 minutes during lunch with a good pump will help protect your milk supply. Store pumped milk in a proper container, and keep it refrigerated until you leave work. Then, take it home in an insulated cooler bag, placing the milk containers so they touch the frozen ice packs in the insulated cooler.
A good approach is to use the fresh milk pumped at work in the next day's bottle feedings. Refrigerate Friday's milk and use it for Monday's feeding. Keep frozen milk available for emergencies, but refresh your frozen milk supply periodically so it doesn't get too old.
Tips For Handling Breast Milk
We've assembled the following tips, from credible medical sources, on four essentials every pumping mother needs to know about handling expressed breast milk:
- How to store it
- How to warm it
- Don't reuse it
- Nutrient degradation when it is warmed too high
How Should I Store Breast Milk?
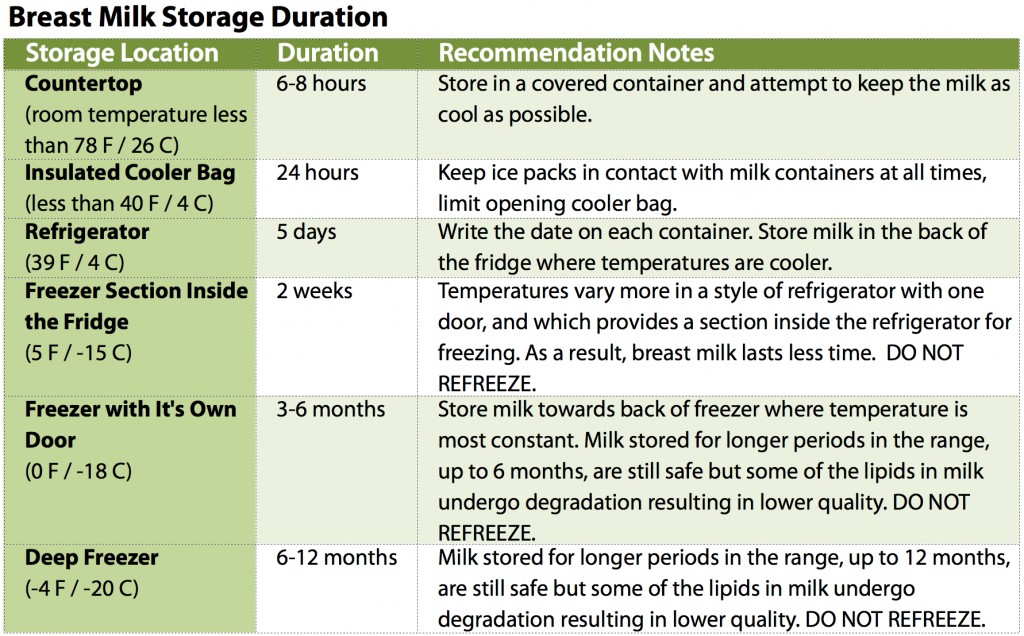
You'll want to store breast milk in a container designed for that purpose. Follow these guidelines to keep your expressed breast milk healthy for your baby:
- Wash hands thoroughly before expressing or handling milk.
- The color of milk will vary depending on mom's diet. Don't worry. This is normal.
- Use clean containers and pumping equipment that have been washed in hot, soapy water and rinsed thoroughly. (Boiling items after washing is important where the water supply may not be clean. If this is the case, BabyGearLab recommends using shatterproof glass containers.)
- Hard containers with an airtight seal are preferred for long-term storage of human milk, such as glass. Do not fill the container completely because breast milk expands as it freezes.
- Plastic storage bottles and bags specifically designed for human milk storage can be used. Do not use ordinary plastic storage bags or formula bottle bags.
- Several expressions throughout the day may be combined. Keep each day's milk separate from other days.
- Write the date on the container, so you can always use the oldest milk first.
- Do not add fresh breast milk to already frozen milk. It is best not to mix the two.
Once you have breast milk in a sealed container, you will want to consider whether to refrigerate it or freeze it. Here are some guidelines:
- For milk that will be used the next 1 to 3 days, it is best to refrigerate it
- Store refrigerated fresh milk in the back of the main body of the refrigerator where it is the coolest.
- Use the date you write on each container to use the oldest milk first, and make sure you use refrigerated milk within 5 days (ideally sooner)
- Breast milk will separate b/c it is not homogenized. The cream will rise to the top. Before feeding, gently swirl the container to mix the cream back through, do not shake vigorously.
- Keep a supply of frozen milk on hand for emergencies, or to store extra production
- Refresh your frozen supply periodically, using the older frozen milk, and freezing a fresh supply
- When freezing, store milk toward the back of the freezer, where the temperature is the most constant.
- Appropriately stored frozen breast milk smells and tastes different than fresh, but is fine as long as baby will accept it.
How Should I Warm Breast Milk?
We recommend thawing overnight in the refrigerator the amount of frozen breast milk you expect to use the next day. Thawing frozen milk in the fridge will shorten warming time, thus avoiding an extended period of time with a hungry, impatient, and crying baby.
Then, warm thawed milk by holding the bottle under warm running water to quickly thaw. Do not use hot water to thaw milk, lukewarm will do the trick. You can also place the sealed container in a bowl of warm water for 20 minutes to bring it to body temperature. If you did not pre-thaw the frozen milk in the refrigerator, you can use these same approaches, but again, avoid the temptation to use hot water to warm up milk.
The key to warming breast milk while preserving its full nutritional value is to avoid overheating. Your goal is to heat breast milk to approximately at or a bit below body temperature (98.6 F / 37 C). That is really just luke warm water, not hot. Using only warm water bath temperatures to heat up milk will avoid the loss of nutrients and the risk of overheating.
Avoid using a microwave oven to thaw or heat bottles of breast milk. Microwave ovens do not heat liquids evenly. Uneven heating could easily scald a baby or damage the milk. In addition, bottles may explode if left in the microwave too long. And, the excess heat can destroy the nutrient quality of the expressed milk.
A Word of Caution for Bottle Warmer Users
Alternatively, you can use a top-ranked bottle warmer to simplify warming. However, we advise caution to avoid overheating breast milk if you use a bottle warmer. If you want to use a bottle warmer, then we recommend the Kiinde Kozii, which won our Editors' Choice award due to its incorporation of a sophisticated system to avoid overheating. The other bottle warmers we tested make it too easy, in our opinion, to expose breast milk to high temperatures, which can result in significant loss of nutritional and/or immunological value.
Tips for Warming Breast Milk
Here are some guidelines to keep in mind when warming breast milk:
- Thawed milk is safe in the refrigerator for 24 hours. DO NOT REFREEZE.
- Use the oldest milk first. Date container at the time of collection.
- Baby may drink milk cool, at room temperature, or warmed.
- Thaw milk by placing it in the refrigerator the night before use or gently rewarm it by placing the container under warm (< 58C) running water or in a bowl of warm water.
- Do not let the level of water in the bowl or from the tap touch the mouth of the container.
- Never use a microwave oven or stovetop to heat breast milk, as these may cause scald spots and will destroy antibodies. A microwave may also destroy valuable nutrients and vitamins in breast milk.
- Swirl the container of milk to mix the cream back in, and distribute the heat evenly. Do not stir.
- Milk left in a feeding container after a feeding should be discarded and not used again.
- Do not refreeze breast milk once it is thawed or partially thawed.
If My Baby Doesn't Finish a Bottle of Breast Milk, Can I Reuse It?
No.
Once baby has completed feeding, discard any remaining breast milk. Do not save milk from a used bottle for use at another feeding.
Can I Damage Breast Milk By Improperly Warming It?
Yes.
A number of scientific studies have been conducted over the last 30 years to investigate how heat can impact the nutritional value of breast milk. As a general rule, all the studies urge that you do not use a microwave or stove-top to warm breast milk, as the damage due to overheating breast milk can be substantial. But some of the studies identify significant loss of breast milk nutritional and/or immunological value beginning at relatively low temperatures.
It may be surprising to learn that even your hottest tap water is probably too hot for breast milk warming. If you use tap water to heat breast milk, use warm water, not the hottest. Most hot tap water is set to 120F to 140F (the Consumer Product Safety Commission suggests that water heaters be set to a maximum temperature of 120F to prevent scalding injuries in children, but many are set higher). Once breast milk is warmed to temperatures higher than 104F/40 C (for perspective, 104F is what most of us would describe as warm, and is the normal limit for hot tubs), breast milk's nutritional and immunological value begins to deteriorate. By the time breast milk reaches sustained temperatures of 125F/52C, which is hot, but not yet scalding, the rate of breast milk quality deterioration increases significantly (for perspective, 140F/60C is what many people would start to consider scalding hot).
The Science of Breast Milk Handling
While at first, these breast milk handling guidelines may seem persnickety, the science behind them leaves no room for interpretation. How a mother handles breast milk can make a real difference in the health and nutrition of her infant. For those interested in learning the medical nitty-gritty behind these guidelines and more can refer to, Breastfeeding: A Guide for the Medical Professional the same book your pediatrician or lactation specialist may be using.
References
- Human Milk Storage Information for Home Use for Full-Term Infants, The Academy of Breastfeeding Medicine, Volume 5, Number, 3, 2010
- American Academy of Pediatrics on storing and preparing expressed breast milk
- Mayo Clinic guidelines for storing breast milk
- Breastfeeding: A Guide for the Medical Professional, Ruth A. Lawrence and Robert M. Lawrence, 7th Edition
- Quan R (et al). Effects of microwave radiation on anti-infective factors in human milk. Pediatrics 89
- Wardell J (et al). Bile Salt-Stimulated Lipase and Esterase Activity in Human Milk after Collection, Storage, and Heating: Nutritional Implications. Pediatric Research. 1984.
- Medela guidelines for collection and storage of breast milk